The Triple Aim: Care, Health, And Cost
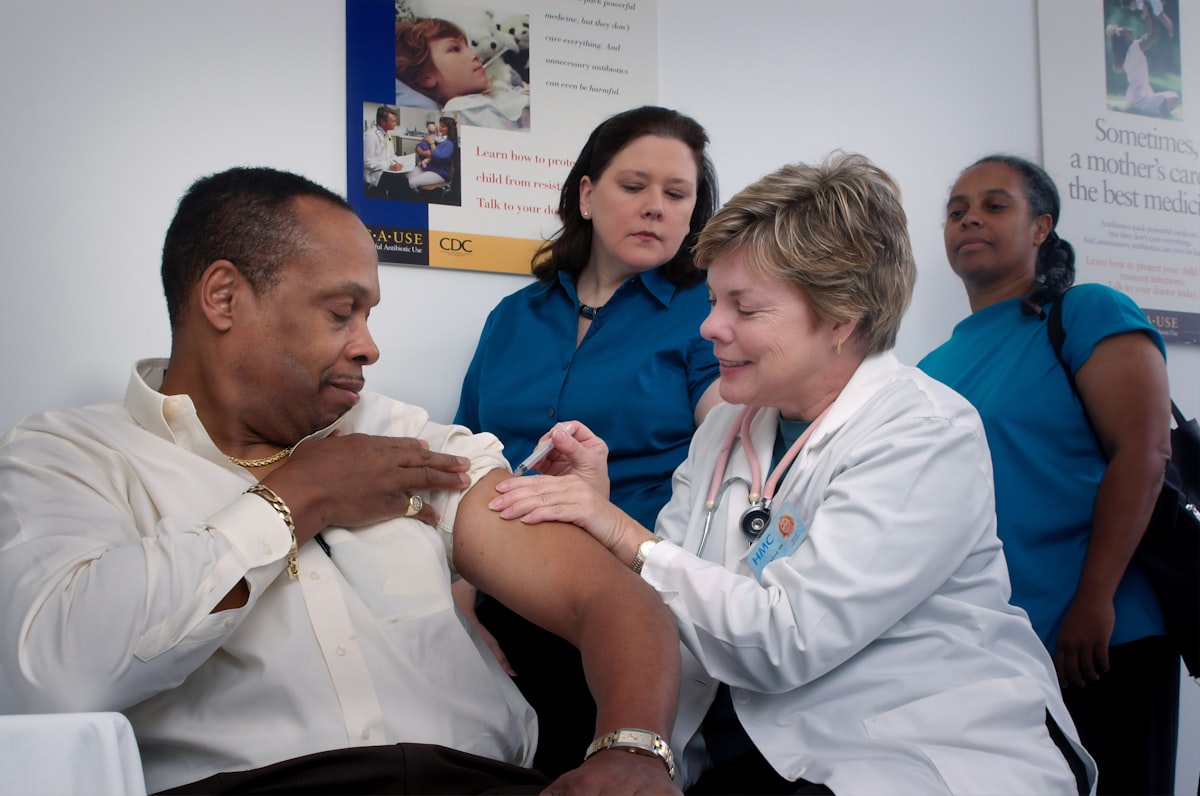
Improving the U.S. health care system requires simultaneous pursuit of three aims: improving the experience of care, improving the health of populations, and reducing per capita costs of health care. Preconditions for this include the enrollment of an identified population, a commitment to universality for its members, and the existence of an organization (an “integrator”) that accepts responsibility for all three aims for that population. The integrator’s role includes at least five components: partnership with individuals and families, redesign of primary care, population health management, financial management, and macro system integration.
The components of the Triple Aim are not independent of each other. Changes pursuing any one goal can affect the other two, sometimes negatively and sometimes positively. For example, improving care for individuals can raise costs if the improvements are associated with new, effective, but costly technologies or drugs. Conversely, eliminating overuse or misuse of therapies or diagnostic tests can lead to both reduced costs and improved outcomes. The situation is made more complex by time delays among the effects of changes. Good preventive care may take years to yield returns in cost or population health.
Pursuit of the Triple Aim is an exercise in balance and will be subject to specified policy constraints, such as decisions about how much to spend on health care or what coverage to provide and to whom. The most important of all such constraints, we believe, should be the promise of equity; the gain in health in one subpopulation ought not to be achieved at the expense of another subpopulation. But that decision lies in the realms of ethics and policy; it is not technically inherent in the Triple Aim.